Caroline Lee-Davey, Chief Executive at Bliss, said: “Our new report shows that ongoing neonatal access restrictions continue to have a serious impact on families. Parents are unable to be with their baby as much as they need to be and some parents – usually fathers and partners – are unable to spend time with or be involved in their baby’s care at all. The implications of this on family bonding and mental health will be felt long into the future.”
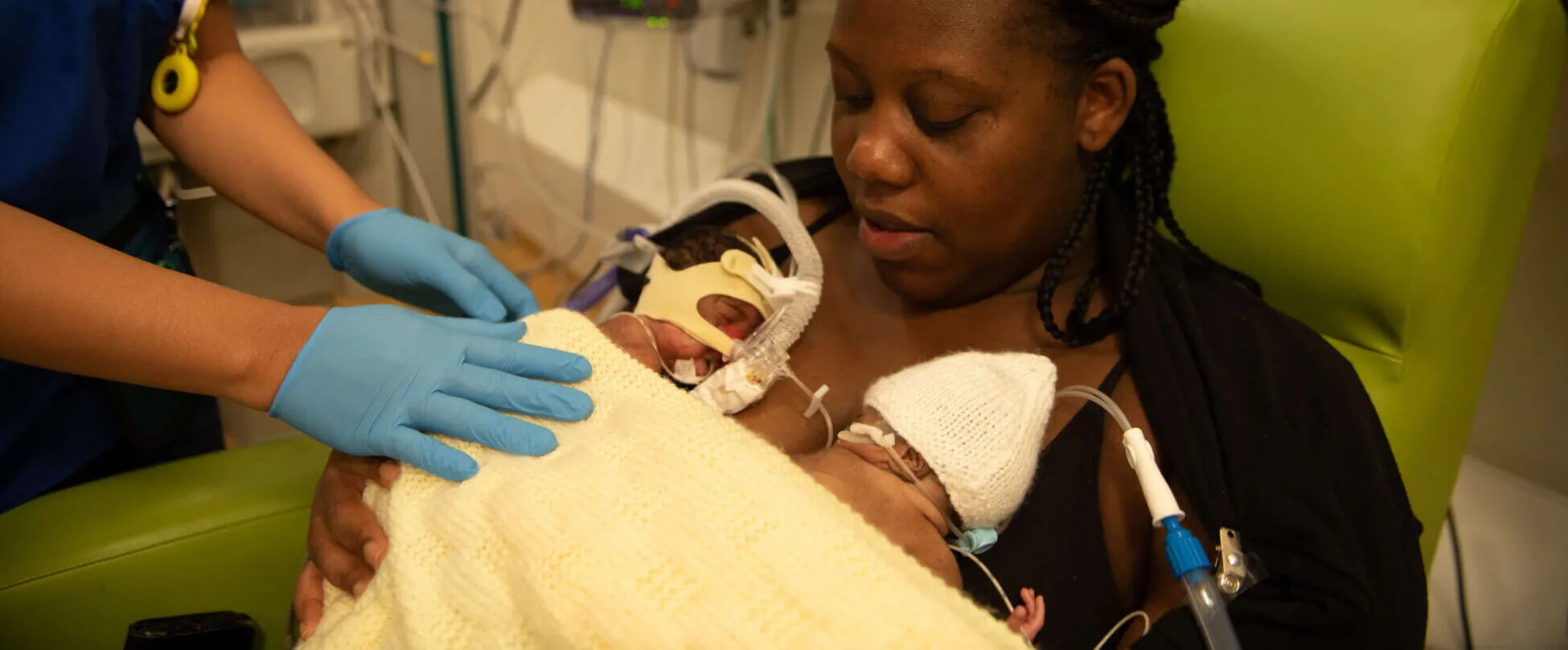
A report by Bliss reveals that ongoing Covid-19 neonatal access restrictions continue to have a serious impact on families
Findings from the report Locked Out: The Impact of COVID-19 on Neonatal Care highlight challenges faced by parents in spending time with their infants in the critical first days and weeks of life, with parents 70% more likely to say they found it difficult to bond with their baby if Covid-19 had resulted in restricted access to the neonatal unit.
The report includes a survey of 70 NHS Trusts and over 500 parents of neonatal babies born between March 2020 and February 2021. Data showed that despite the widespread rollout of Covid-19 testing, only 7 of the 25 units who were testing parents regularly were able to facilitate full 24-hour access for both parents at their baby’s cot-side. Findings from the report indicated that this has had severe negative outcomes for parental bonding, attachment and mental health.