Unicef UK Baby Friendly Initiative’s Programme Director Sue Ashmore shares insight into how the Baby Friendly neonatal standards are revolutionising care for sick and preterm babies, and how Royal Exeter & Devon’s neonatal unit are leading the way in putting these babies and their families at the heart of everything they do.
As a student midwife in the 1980s, I remember standing at the door of our neonatal unit and counting to 10 before I could steel myself to press the buzzer and ask to be let in. Once in, I never knew how to attract the attention of the busy and important looking staff gathered around the bewildering array of machinery, and I was often told to ‘move out of the way’ as I feebly tried to deliver my errand. I don’t remember seeing many parents in this intimidating environment.
Fast forward 30 years and I am standing with parents and staff in the first ever Unicef UK Baby Friendly accredited neonatal unit, looking at the future, but also drawing a thread back to all those who have ever stood on the threshold of a neonatal unit willing themselves not to flee. The Baby Friendly neonatal standards were launched in 2015 and all those years later, were still partly based on the testimony of parents and professionals confessing in anonymous interviews to feelings of fear, alienation and ‘being in the way’ on many different neonatal units up and down the country.
Bringing parents into the heart of neonatal care
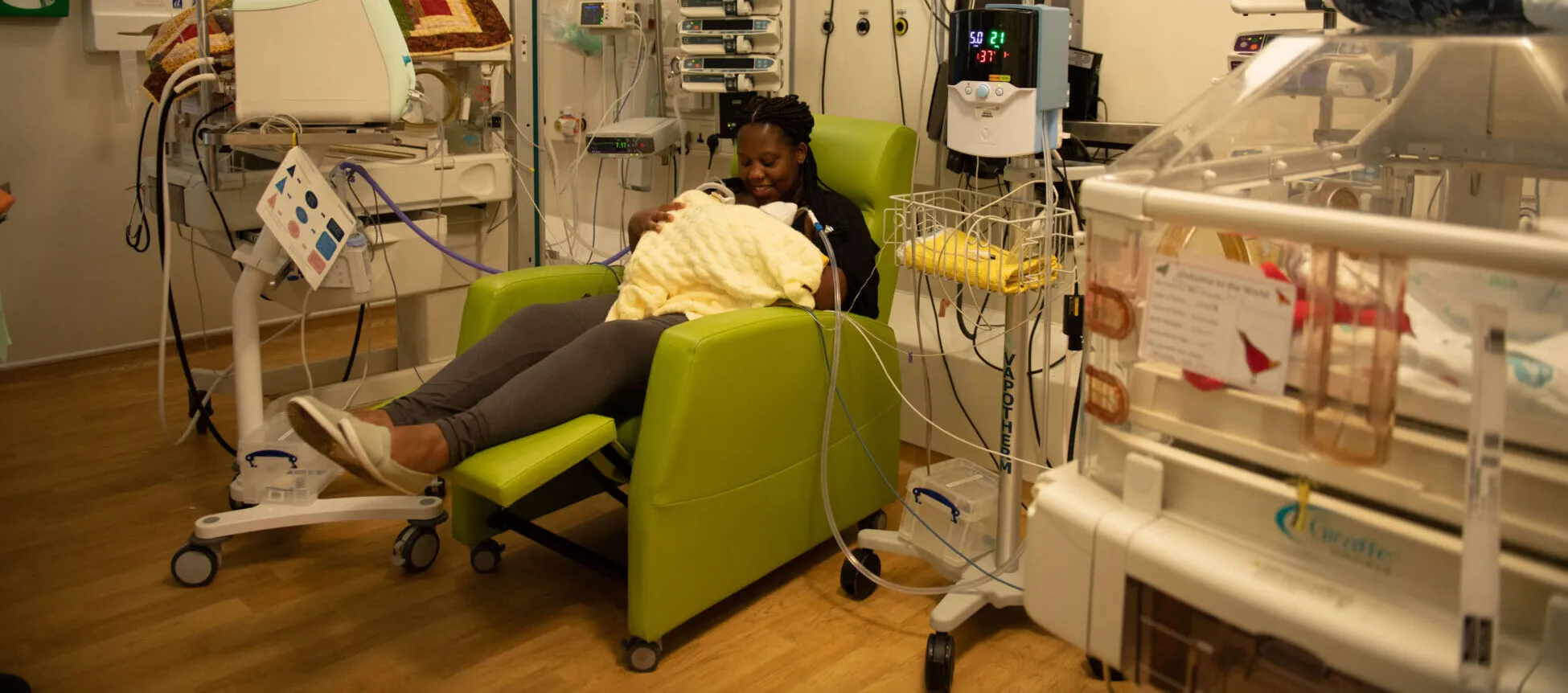
Exeter is a world away from these feelings. Standing here, the words that spring to mind are kind, reassuring, calm. Parents are sat in comfortable armchairs or laid on camp-beds, cups of coffee in hand as smiling staff offer quiet support. Babies are nestled in skin contact or are gently touched as parents carry out care. There are rooms with sofas and dimmed lights for those needing time out, a kitchen to prepare food and drink and a crèche area for young siblings to play.
I am here with Unicef UK president, TV and radio presenter Kirsty Young (she of the beautiful voice on Desert Island Discs) and the TV producer of the brilliant ‘Call the Midwife’, Dame Pippa Harris. I am desperate to impress upon them that this is not a typical unit, and that what they are seeing is revolutionary. However, I am not being helped by the unassuming staff and parents telling their stories with such understatement and modesty. There is the matron confessing that there was ‘some’ resistance to changes at the start, and the consultant who shrugged when asked about 24 hour parental access, stating that it’s quite easy once you get used to it and really great to work with parents. There is the young mother of the 15 month old, born at 24 weeks, who never left her baby’s side for the 111 nights she was on the unit and who only ever gave her daughter breastmilk, before eventually going home exclusively breastfeeding. When asked how she managed, she observed that it was fine and would have been much worse if she had had to leave her baby. Her daughter, bright as a button and running around, showed absolutely no outward signs of her extreme prematurity.
Why is Exeter so far ahead of the game, and do they have a formula that others could follow? As the conversation flowed, it became obvious that they did. They are determined to implement the Baby Friendly standards – all of them, all of the time. The standards are built around a holistic, child rights based assessment of what a baby needs alongside the clinical care to survive. These babies desperately need to build close and loving relationships with their family and to receive the best possible nutrition to survive and grow. If they are to have this, they also need to have high quality time with their parents, not just for a few hours a day, but for as much of the time as possible.
The role of Baby Friendly
Baby Friendly provides a roadmap for units to make this happen – comprehensive standards, education, internal audit and external assessment. The comprehensive nature of the standards, the requirement that it is for all babies and includes all staff, as well as the rigour of the internal audits and external assessments carried out by health professional Unicef staff, mean that Baby Friendly accreditation is the pinnacle of achievement for any unit working to improve families’ experiences of neonatal care.
With Baby Friendly it is not possible to pick and mix which standards to implement depending on particular staff interests or on what is culturally acceptable at the present time. Tough decisions have to be made, resistance addressed and all staff and parents fully involved in the changes required. It is very challenging and can seem daunting at the start, but it is worth it as an investment in the future of the UK’s most vulnerable sick and preterm babies. Only by taking this holistic and rigorous approach can services get the depth and breadth of change that is occurring in Exeter, and it is this that is needed, if these babies are going to have the secure family attachments and optimal nutrition to enable them to survive and thrive into the future.
Making “special” care the norm
As we were leaving Exeter, Kirsty asked the Infant Feeding Lead ‘what next?’ She thought for a moment and then said that it broke her heart when babies were transferred to other units and parents begged to stay because of the ‘special’ care in Exeter. ‘It shouldn’t be special’ she said, ‘it should be ordinary. We have to get out there and persuade every unit to go Baby Friendly, and create a new normal’.